Regenerative Medicine and Burn Treatment
This was the focus of the International Symposium on Regenerative Medicine. The event, organized by the Medical University of Pleven, brought together leading specialists, with Dr. Nikolay Tsaribashev participating as a panelist by invitation.

Leading specialists in regenerative and translational medicine presented the latest developments in tissue repair.
Alongside fundamental scientific advances, the discussion also highlighted the growing practical application of innovative technologies. New injectable biocompatible materials for vascular treatment in oncology were presented. A strong focus was placed on the treatment of severe burns-from 3D printing of human skin to the use of autologous growth factors and stem cells.
Participation of Dr. Nikolay Tsaribashev
During the symposium, Dr. Tsaribashev presented the approaches of Regenics Medical in the treatment of patients with burns. This reflects the core direction of Regenics Medical—developing and applying tissue-regenerative methods to support human health and longevity.
You may already be familiar with our joint work with PFC Levski in the treatment of Svetoslav Dimitrov, a youth football coach who sustained severe burns. Our shared goal with PFC Levski and burn centers across the country is to identify ways to integrate tissue-regenerative technologies into routine clinical practice. This would allow more patients with severe burns to access advanced treatment options.
In parallel, we are discussing the initiation of research aimed at developing standardized protocols for the treatment of severe burns.
Below is a scientific overview of the presentation, outlining the methods used and the results achieved.
Burn Treatment and Regenerative Approaches: From Clinical Practice to Scientific Development
We will keep you informed about all developments in this field. If you are not yet subscribed to our newsletter and would like to stay updated on health, longevity, and well-being, you can sign up here.
Scientific Overview of the Presentation. (Abstract)
The following text presents the clinical approach shared by Dr. Tsaribashev during the symposium. It summarizes the methods used, the observed outcomes, and the role of regenerative therapies in the treatment of severe burns.
Multimodal Therapeutic Approach in Burn Treatment: The Role of PRGF, Photobiomodulation, and Cold Atmospheric Plasma
Author
Dr. Nikolay Tsaribashev, MD, PhD
Introduction
Burns represent a significant global healthcare burden and are often complicated by infections, delayed healing, and scar formation. Conventional treatment includes surgical debridement (removal of damaged tissue), antimicrobial therapy (often antibiotics that may disrupt the microbiome and local immune response), and skin grafting.
Emerging tissue-regenerative therapies aim to improve tissue repair. Plasma rich in growth factors (PRGF), photobiomodulation (PBM), and cold atmospheric plasma (CAP) have gained attention due to their strong regenerative, anti-inflammatory, and antimicrobial properties. This study presents the effectiveness of these methods in the treatment of burns through a clinical case example.
Methods
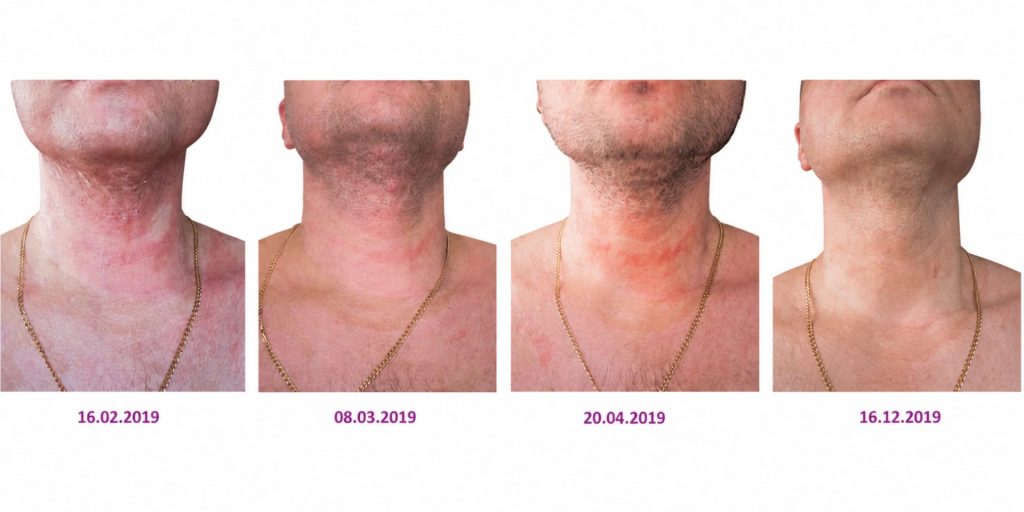
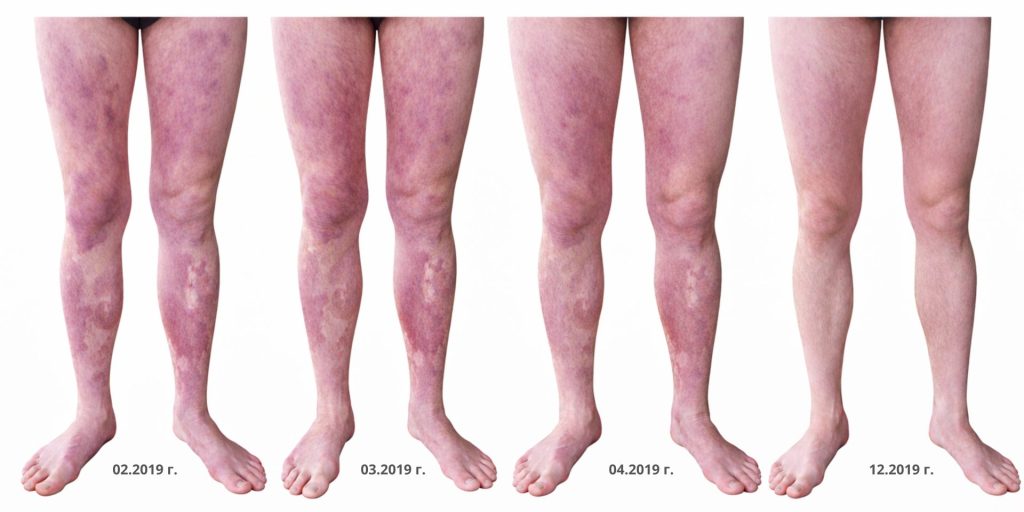
A patient with severe burns affecting 70% of the total body surface area, classified as IIA and IIB according to the modern classification, was treated over a period of 10 months using all three methods.
Results
PRGF supports wound healing through the controlled release of growth factors such as vascular endothelial growth factor (VEGF), platelet-derived growth factor (PDGF), and transforming growth factor-β (TGF-β). These factors stimulate cell proliferation and epithelialization (the restoration of intact skin and closure of the wound after a burn).
PBM demonstrates significant efficacy in accelerating burn wound healing by activating endogenous TGF-β1 signaling, reducing inflammation, and exerting antibacterial effects, while also enhancing cell proliferation and tissue remodeling (the organization of healthy tissue).
CAP exhibits strong antimicrobial effects and effectively reduces bacterial load without disrupting the microbiome or interfering with tissue regeneration, thereby overcoming one of the key limitations of conventional antiseptics.
In addition, CAP has been shown to enhance wound closure and promote regeneration of the skin and subcutaneous tissue by activating resident stem cells and epidermal cells (the outer layer of the skin). This leads to increased levels of growth factors such as TGF-β1 and connective tissue growth factor (CTGF).
Combined, these therapies contribute to improved healing progression, effectively suppress infections, and enhance the quality of newly formed tissue, as demonstrated in the presented case. In this patient, the multimodal treatment led to complete resolution of burn-related signs and prevented fibrosis (the formation of tissue that disrupts the integrity and function of the skin).

Conclusion
PRGF, photobiomodulation, and cold atmospheric plasma represent promising complementary therapies in the treatment of burns. Their synergistic action-combining regenerative stimulation, anti-inflammatory modulation, and antimicrobial activity offers significant advantages over conventional treatment methods. Further large-scale clinical studies are needed to standardize protocols and confirm long-term efficacy and safety.



